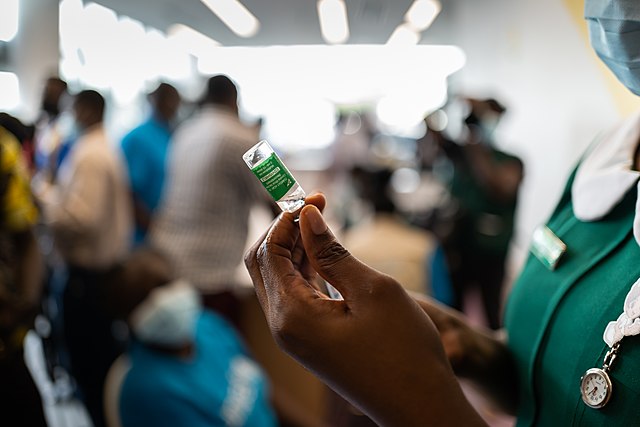
A nurse prepares to administer a dose of the AstraZeneca/Oxford COVID-19 vaccine at Accra’s Ridge Hospital, as Ghana began to roll out its national COVID-19 vaccination campaign, March 2021. Photo by Nana Kofi Acquah via Wikimedia Commons.
COVID-19 vaccine inequality remains, despite many of us returning to a form of ‘normality.’ Kai Evans finds out why.
The COVID-19 pandemic has had a devastating impact on communities all over the world, but the distribution of vaccines has, at least in the Global North, seen restrictions being rolled back and for many, there is a sense that ‘COVID-19 is over’. However, the distribution of vaccines has been uneven, and for large amounts of the global population, the COVID-19 pandemic is anything but over. This inequality in vaccine access threatens to prolong the pandemic, allow new, potentially more dangerous variants to emerge and have long-lasting consequences for the most vulnerable communities.
Initially, vaccine nationalism and a focus on securing vaccine supplies for wealthy countries resulted in many countries in the Global South being left behind. Now, thankfully, many regions of the Global South, such as Latin America and much of Asia, have made significant gains in both purchasing and distributing vaccines. However, there is one region that continues to struggle in this regard: Africa.
As of 5th March 2023, over 80% have received at least one dose in Latin America, the Asia-Pacific region and USA and Canada. This number falls to 70% in Europe, with the Eastern section of the continent having difficulties. The Middle East has vaccinated 59% of their population with at least one dose. How much of the African population have received a vaccine?
37%.
Some countries in Africa, such as the Democratic Republic of the Congo, Cameroon and Senegal have vaccination rates (for one dose) of just 13%, 13% and 16% respectively.
This disparity in vaccine distribution led to calls for an equitable distribution of the vaccine, with organisations such as the World Health Organization (WHO) and the World Bank leading the charge. However, in 2023, the problem of vaccine equality has been and continues to be multi-faceted, with vaccine purchasing, vaccine distribution and vaccine hesitancy at the top of the list of challenges.
Vaccine purchasing
One of the main challenges facing countries in the Global South initially was a lack of funds to purchase vaccines. The cost of purchasing vaccines is high, and many of these countries do not have the resources to secure large quantities of vaccines. This has led to a reliance on initiatives such as the COVAX Facility, which aims to ensure that all countries, regardless of their income level, have access to safe and effective vaccines. While the COVAX Facility has faced challenges in securing and distributing enough vaccines to meet demand, it has been an invaluable resource to the lowest-income countries and the most vulnerable communities.
As of February 2023, over a billion vaccines have been delivered to African nations, through a combination of COVAX, AVAT (African Vaccine Acquisition Trust), donations, and bilateral and multilateral agreements. This is certainly not an insignificant number, but given the African population stands at approximately 1.3 billion, it is clearly not enough to even give everybody one dose, never mind two.
Meanwhile, the USA alone has acquired 1.08 billion vaccines, for their population of approximately 335 million. In other words, there is enough for about 3 doses per person.
Vaccine distribution
Despite the clear vaccine inequality in terms of purchasing power and the reliance this brings on donations and facilities such as COVAX, the numbers don’t add up. If all of the vaccines delivered to Africa were used, one would expect approximately 80% of the African population would have received a first dose, or 40% would be fully vaccinated. Instead, just 37% have received a first dose, with approximately 30% being fully vaccinated.
Clearly, there are also logistical challenges to overcome in Africa. Many of these countries have limited health infrastructure and face challenges in storing and distributing the vaccines. This can result in vaccine wastage and a slower pace of vaccination. For example, Project HOPE, a non-profit working to overcome global health challenges, found that a lack of funds and a lack of trained professionals were key contributing factors to the low vaccination rates in Africa. A similar insight is shared by Adam Bradshaw, senior coronavirus adviser at the Tony Blair Institute for Global Change (TBI) and former adviser to New Zealand’s vaccine policy:
‘A lot of vaccine workers will travel 10 hours, pay for it with their own money – for their fuel, accommodation, food and the rest. But that’s not a sustainable model. You wouldn’t expect that in a high-income country and we shouldn’t expect it in a low-income country either.’
This issue is particularly compounded in the poorest areas, which are often rural, and thus are often lacking trained professionals and require significant travel time, and cost to reach.
In the early stages of the vaccine rollout, there were other logistical issues related to donations. Vaccines tended to only be donated when countries in the Global North were certain they did not need them. Therefore, by the time they reached Africa, they were often extremely close to their expiry date, and governments had very little time to mobilise resources and organise vaccination campaigns. As a result, since 2022, John Nkengasong, director of the Africa Centres for Disease Control and Prevention, has led calls that any donations come with at least a three-month shelf life.
Vaccine hesitancy
There is also a lack of trust in the vaccine in some communities, which has led to vaccine hesitancy and a slower pace of vaccination. People from countries in Africa have been subject to the same conspiracy theories and misinformation seen here, in Ireland, and around the world.
According to experts such as TBI policy associate Liya Temeselew, who works on coronavirus policy in Ethiopia, this has been compounded by the ‘unfair’ manner in which vaccines have been distributed:
‘If you see in the news that the vaccines coming to your country are nearing their expiry date, the perception of this isn’t particularly great.’
In addition, the unreliability of vaccine availability ‘undermines the credibility and confidence in vaccines.’

Reasons for hope
Despite these challenges, there are reasons for hope. Other countries in the Global South have made significant progress in vaccinating their populations, despite slow starts. For instance, India has launched a massive vaccination campaign and has fully vaccinated 70% of their population. Similarly, countries in Africa, such as Rwanda (78%), Liberia (76%) and Morocco (64%) have made significant progress in fully vaccinating their populations and have used innovative approaches such as door-to-door campaigns to reach remote communities. Rwanda in particular can act as an example to other countries in the region. They devised a strategy early, buying 437 new refrigerators as well as refrigerated vehicles to store and transport vaccines, even prior to their arrival. This enabled an efficient and reliable vaccine rollout which, along with open and honest communication from the government, kept trust levels high and vaccine hesitancy low.
In conclusion, the COVID-19 pandemic has highlighted the need for an equitable distribution of vaccines globally. The disparity in vaccine distribution in the Global South, and particularly Africa, threatens to prolong the pandemic and have long-lasting consequences for vulnerable communities. It is imperative that wealthy countries step up and support initiatives such as the COVAX Facility to ensure that all countries have access to safe and effective vaccines. As the WHO has frequently said, ‘No one is safe, until everyone is safe.’ It is only through a concerted global effort that we can overcome this pandemic and build a more equitable and resilient world.